Health Panel Calls for Routine Anxiety Screening for Adults
This article is from RISQ Consulting’s Zywave client portal, a resource available to all RISQ Consulting clients. Please contact your Benefits Consultant or Account Executive for more information or for help setting up your own login.

The U.S. Preventive Services Task Force (Task Force) recommends that adults under the age of 65 get regularly screened for anxiety. The draft recommendation applies to adults 19 and older who don’t have a diagnosed mental health disorder. It’s meant to help primary care clinicians identify early signs of anxiety, which can go undetected for years. This is the first time the Task Force has recommended anxiety screening in adult primary care without symptoms.
The Task Force, a group of independent disease prevention and medical experts, defines anxiety disorders as “characterized by greater duration or intensity of a stress response over everyday events.” Recognized types include generalized anxiety disorder, social anxiety disorder and agoraphobia.
The draft recommendation noted that the lifetime prevalence of anxiety disorders in adults in the United States is 40.4% for women and 26.4% for men. The recommendation was prioritized due to anxiety’s public health influence and the country’s increased focus on mental health in recent years.
“Our hope is that by raising awareness of these issues and having recommendations for clinicians, that we’ll be able to help all adults in the United States, including those who experience disparities.”
-Lori Pbert, Task Force member
The guidance stops short of recommending anxiety screening for people 65 and older since many common symptoms of aging—such as trouble sleeping, pain and fatigue—can also be symptoms of anxiety. The Task Force said there wasn’t enough evidence to determine the accuracy of screening tools in older adults to distinguish between anxiety symptoms and conditions of aging.
The Task Force advised clinicians to use their judgment in discussing anxiety with older patients. It also reiterated an earlier recommendation that adults of all ages undergo routine screening for depression.
What’s Next?
The proposed recommendation is not final and is in a public comment period through Oct. 17. This is an opportunity for the public to provide their input and perspectives for the Task Force to consider for its final approval.
The Task Force emphasizes that if you already show signs or symptoms of anxiety, you should be assessed and connected to care. Anxiety screening tools, including questionnaires and scales, have been developed and are available in primary care. If you have concerns about anxiety, contact your doctor.
- Published in Blog
Suicide and Crisis Lifeline Help for Alaskans
By Ashley Snodgrass, Employee Benefits Analyst
As of July 16, 2022, the National Suicide Prevention Lifeline is changing to be more easily accessible. Now help is only a three-digit number (988) away.
According to Alaska Department of Health Division of Behavioral Health, this change has been planned for many years. The goal is to make it easier to connect anyone in distress to “compassionate, accessible support,” including trained crisis counselors.
I’d like to highlight some statistics that support why this hotline is needed. These are taken directly from the State of Alaska’s FAQ about the new 988 hotline:
“Alaska and the nation are experiencing a mental health crisis. But the crisis is not irreversible.
- In Alaska in 2020, suicide was the leading cause of death for American Indian and Alaska Native youth ages 10-19, and for youth ages 10-14. Suicide was the 2nd leading cause of death overall for all Alaska youth and young adults, ages 15-34.
- According to the most recent Youth Risk Behavior Survey in 2019, over 1 in 3 Alaska high school students reported feeling sad or hopeless almost every day for 2 or more weeks in a row; 25% seriously considered attempting suicide; and nearly 20% attempted suicide.
- When fully implemented, 988 will improve Alaska’s system of care that responds to individuals experiencing a behavioral health crisis.
- Those statistics are sobering, but there is good news:
-
-
- Suicide is most often preventable. For every person who dies by suicide annually, there are 316 people who seriously consider suicide but do not kill themselves.
- Over 90% of people who attempt suicide go on to live out their lives.”
-
An FAQ about the 988 Hotline has been made available on the State of Alaska’s webpage, accessible at https://health.alaska.gov/dbh/Pages/Prevention/988/default.aspx#faq
I’ve compiled some additional resources for mental health services in Alaska below:
- Alaska’s Careline: 1-877-266-4357 (HELP) or text “4help” at 839863
- 24/7 free and confidential crisis line
- UAA Psychological Services Center: 907-786-1795
- Telehealth counseling services available at reduced costs to all members of the community.
- Veterans Crisis Line: 1-800-273-TALK (8255) and press 1 or text to 838255, or use Veterans Crisis Chat on the web
- The Veterans Crisis Line is a free, confidential resource that connects veterans 24 hours a day, seven days a week with a trained responder. The service is available to all veterans, even if they are not registered with the VA or enrolled in VA healthcare.
- State of Alaska Behavioral Health Links & Resources
- https://health.alaska.gov/dbh/Pages/TreatmentRecovery/MentalHealth/links.aspx
- Including links to Community Treatment and Recovery Providers with Websites:
In case of emergency, always call 911 or go to your nearest emergency room for treatment.
- Published in Blog
Mental Health in the Workplace
By Alison Nelson, Sales and Marketing Coordinator
Last week, Naomi Osaka, a world-renowned tennis player, withdrew from the French Open. Why would she withdraw from such an important match, resulting in a $15,000 fine? The answer is simple: mental health.
Naomi Osaka explained that she struggles with depression and anxiety and needed to put her health first. Unfortunately, critics were quick to label Osaka a “diva” or even a “special snowflake”. While most of the world applauded Osaka’s stand, and the mediation app, Calm, even offered to pay the fines for any tennis players who skip media appearances due to mental health, the initial critics provided an alarming reminder of the stigma surrounding mental health.
According to the World Health Organization (WHO), an estimated 264 million people suffer from depression and many of those people also have anxiety. WHO also states that depression and anxiety disorders cost the global economy one trillion U.S. dollars each year in lost productivity. Despite the staggering amount of people who have depression or other mental illnesses, and as the Osaka critics demonstrated, the negative stereotypes about mental health are alive and well. Yet, it is because of this stigma that employers can’t afford to stay silent.
Not only is there a direct correlation between mental health and productivity, but according to this article:
- Employees with untreated mental health conditions use nonpsychiatric health care services 3 times more than those who do get treatment.
- Mental illness is the single greatest cause of worker disability worldwide.
- 62% of missed work days can be attributed to mental health conditions.
- Turnover rates are higher for depressed employees, who are 20% to 40% more likely to become unemployed because of their condition.
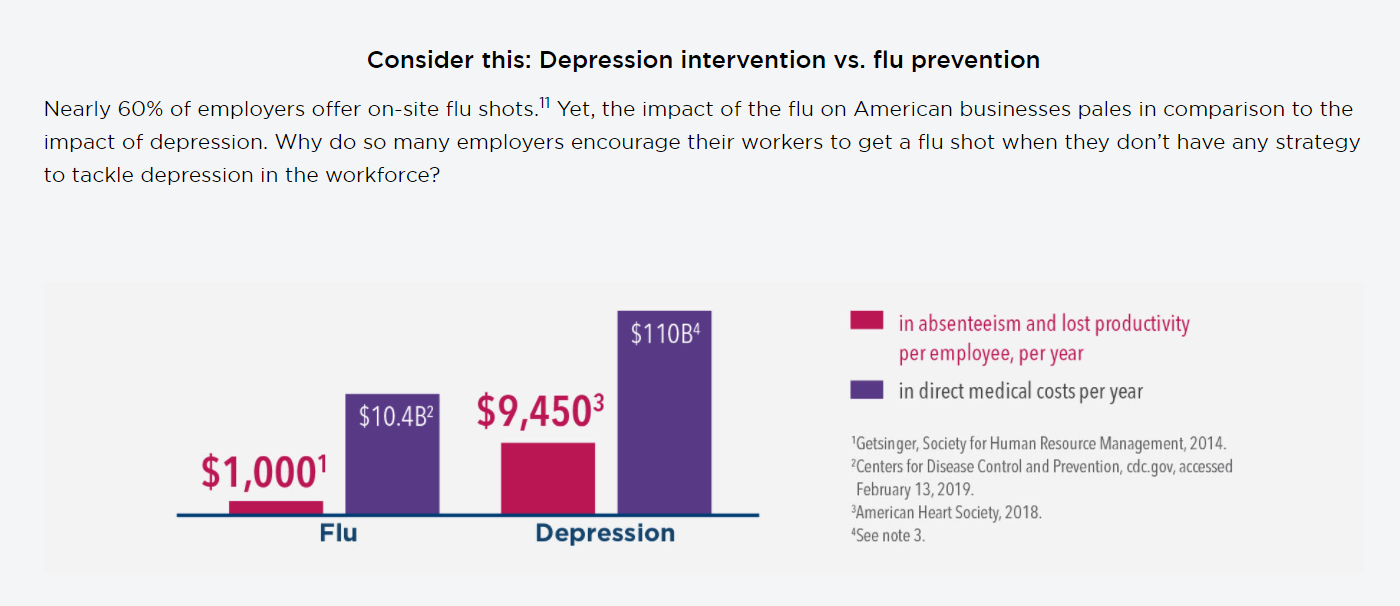
Below is an image from Kaiser Permanente displaying the cost different between flu prevention and depression intervention.
The cost alone should incentivize employers to make an effort to destigmatize mental health, but how should you go about it? Below is a list from LifeSpeak of 10 ways employers can improve mental health in the workplace and you can read the full LifeSpeak article here.
- Speak candidly about mental health. The first step to beating the stigma is to stop treating mental illness as taboo. Whether it’s an article you read, a show you watched, or a personal experience you had, talking about it openly and without shame will help others realize they aren’t alone.
- Keep the conversation going. Workplace culture must be nurtured, which means you can’t just mention mental health once and expect it to catch on. Find multiple opportunities to incorporate the subject into your employees’ day so it stays top-of-mind.
- Include all levels of staff. Your employees won’t believe that you genuinely care about their well-being unless every manager and executive also demonstrates the importance of mental health.
- Encourage employees to take mental health days off. If you still require your employees to provide a doctor’s note or otherwise “legitimate” reason for missing work, it might be time to stop. Part of preventative health involves giving your mind and body a break every now and then, and allowing your staff to miss work in order to recharge can help them stave off more serious health issues down the road.
- Pay attention and be ready to help. If you do notice an employee behaving differently (ex: irritability or low mood), don’t hesitate to ask them if everything is alright. Even if they tell you they’re fine, remind them that you’re there to help and that they have access to assistive resources.
- Make sure the tools and resources are relevant. No matter how much information you supply your employees, it’ll never do any good if it’s outdated or irrelevant. In fact, it might even do harm. Frequently audit your mental health resources to make sure they’re accurate, up-to-date, and contain practical advice that your employees can use to get better.
- Facilitate access to these resources. Similar to the previous point, your staff won’t get much use out of the information if it’s difficult for them to find. Eliminate barriers to access by providing the content in a variety of formats (audio, video, written, etc.), and minimizing the number of steps it takes for them to find it.
- Prioritize confidentiality and anonymity. Even though mental health might be normalized in your workplace, some people might still feel uncomfortable discussing it, particularly if they struggle with addiction, trauma, or suicidal thoughts. Reassure your staff that their privacy is your top concern, and that their use of mental health resources will never be monitored or tracked.
- Design a mentally healthy work space. It’s important for your employees to feel energized and uplifted by their work environment. Research has shown productivity, engagement, and overall wellness increase when people feel comfortable in workspaces with natural lighting, plants, and other positive features.
- Focus on the positive. Mental illness is a serious issue, but it can still be addressed in a way that makes people feel understood, appreciated, and hopeful. Always remember to leave your employees feeling like they have a clear plan of action ahead and that they or their loved ones can get well.
Need more ideas for promoting mental health in your place of work? Click the links below to view additional resources.
CDC– Mental Health in the Workplace
Forbes– Mental Health In The Workplace: A Look At Leaders’ Top Priorities
National Alliance of Mental Health– The Mental Health Movement in the Workplace
- Published in Blog